In small bowel imaging, distention is the name of the game. Unfortunately, in order to get the desired bowel distention for imaging, patients must ingest a large volume of fluid: usually 1350 – 1500ML, approximately 44 – 51 fluid ounces, within a 45 minute time-frame.
It is important to keep in mind that patients undergoing this exam are suffering from inflammatory bowel diseases (Crohn’s, ulcerative colitis) and present with symptoms such as cramping, bloating, diarrhea, constipation, nausea, fatigue, pain and decreased appetite. As a result, many of these patients have a difficult time complying with drinking protocols.
Viscosity affects willingness to drink
To complicate matters, many patients in enterography are instructed to drink a 1% barium sulfate suspension with a viscosity of 80.5cP in order to distend the small bowel.
Viscosity is a measure of a fluid’s resistance to flow. The higher the viscosity, the more resistant to flow a fluid will be. For comparison purposes, water, arguably the most drinkable fluid for humans, has a viscosity of .899cP. A fluid with a viscosity of 80.5cP has a viscosity closer to light-weight cooking oils – corn oil has a viscosity of 72cP, olive oil a viscosity of 84cP (see chart below):
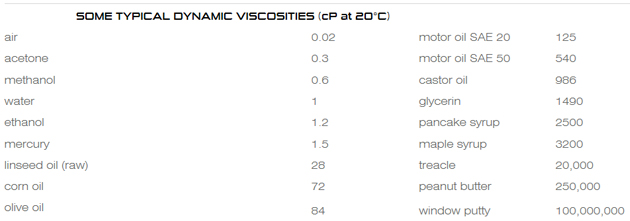
Despite the availability of flavored versions and flavoring agents, the viscosity of the barium sulfate solution makes it hard for patients to drink. Imagine being asked to drink a quart or more of corn oil!
For many patients, the experience of the prep makes them unwilling to repeat the drinking protocol for future exams, which they, unfortunately, have to routinely undergo due to their chronic condition.
Why not just plain water?
The same volume of water does provide adequate soft tissue contrast in enterography, and is well tolerated by patients. The drawback to using plain water is that it is absorbed quickly by the small bowel wall which can result in inadequate luminal distention, especially in the terminal ileum. Additives such as sugar alcohols (e.g.sorbitol, mannitol) and thickening agents (e.g. bean gum, xantham gum) help trap the fluid in the lumen and provide superior distention.
Evaluating an alternative beverage
A group of physicians and clinicians representing the divisions of radiology, gastroenterology, and biostatistics at the Mayo Clinic (Rochester, NY) presented their findings from an evaluation1 of patient tolerance, efficacy, and willingness to repeat the drinking protocol with a flavored beverage for neutral abdominal imaging in the May 2016 issue of the American Journal of Roentgenology.
A non-carbonated, sugar-free, gluten-free beverage with no active ingredient, the flavored beverage evaluated contains sugar alcohols and thickening agents for flavor, emulsion stability, and “mouth-feel." It has a light lemon-lime flavor and a viscosity of 10.5cP.
The researchers found that the flavored beverage scored significantly higher in taste, ease of drinking, and willingness to repeat the drinking protocol than the barium sulfate solution.
They go on to conclude that a drinking protocol for enterography that patients can, and will continue to comply with would have a positive effect on patient satisfactions and consistent quality of exams.
To learn more about this study and the flavored beverage evaluated, contact Beekley Medical at 1-800-233-5539 or info@beekley.com
1 Flavored beverage product for testing and funding for this study was provided by Beekley Medical
Related articles:

Mary Lang
Director of Marketing Communications