The American College of Radiology (ACR), recently, amended their Practice Parameters for the Performance of Screening and Diagnostic Mammography with a recommendation that:
“Facilities should require consistent use of radiographically distinct markers to indicate palpable areas of concern, skin lesions, and surgical scars. In addition, there should be an indication of the type of underlying lesion denoted by each marker, either as a permanent annotation on the appropriate mammographic image(s) or as a description in the mammography report (18). It may be helpful to record such findings on the patient’s intake sheet and/or technologist worksheet.” (Revised 2018 (Resolution 35) section E, labeled Markers, part 2, page 5)
 We reached out to Dr. Michael Linver, a renowned breast radiologist who has committed his career to the mission of mammography and the pursuit of improving patient outcomes, for more insight into this organization, his experience over the years and his thoughts on this recent change.
We reached out to Dr. Michael Linver, a renowned breast radiologist who has committed his career to the mission of mammography and the pursuit of improving patient outcomes, for more insight into this organization, his experience over the years and his thoughts on this recent change.
Based on the ACR’s new language regarding skin markers, we asked Dr. Linver why the use of radiographically distinct skin markers - and particularly, why the use of the distinct shapes is so important in today’s world of breast radiology.
“I am pleased to see the stronger wording regarding the use and documentation of breast skin markers for important clinical findings.
“Because skin markers are now being utilized for various reasons (location of a scar from previous surgery, location of a palpable lump, location of the nipple and skin lesions, etc.), different shapes to reflect these differences become increasingly important.
"For instance, if there are two areas of clinical concern in the same breast, and identical skin markers were applied to both areas, then localization of each separate region on the mammogram could be compromised, and the wrong marker applied to the wrong lesion. This could lead to incorrect characterization of the areas of concern on the mammogram, potentially allowing cancer or cancers to be missed.
"Their proper use can often dramatically affect the interpretation and eventual outcome of the patient’s examination. For example, if skin markers are not properly applied over the area of a palpable breast lump, proper attention might not be given to the area of the lump and its correlation on the mammogram, and a subtle cancer could be overlooked as consequence, potentially allowing a fatal cancer to go undetected."
When asked how the ACR has impacted Dr. Linver in his role as a radiologist over the years he responded:
“The ACR has always been the voice of the radiologists in this country and has been active both professionally in helping radiologists meet the highest possible medical standards, and politically in maintaining the visibility of radiology to government regulators and to the media.
"These roles have become increasingly complex over the 40 plus years I have been a member of the ACR, but the ACR has always risen to the occasion, and has kept radiology the vital force that it enjoys in the medical world. ACR leadership has added multiple branches to address continuing medical education, fundraising, political lobbying, leadership training, and a host of others along the way.
"The ACR continues to look out for my best interests by providing quality educational opportunities through their unique Education Center, allowing me to continue to grow professionally. Such learning opportunities have kept me apprised of the cutting-edge advances in radiology, directly translatable to better care for the patients whose studies I interpret.
"At the same time, the lobbying efforts of the ACR have resulted in greater understanding by the legislature of Radiology's ever-increasing role in modern medicine. As a result, I am better able to work with third party payers in providing the appropriate examinations to the patients we serve.”
Dr. Linver shared his perspective on what is most important when establishing a standard protocol in a breast center:
“First, I must assess the physical capability of my breast center to efficiently perform the various steps of a potentially new protocol. Second, I must be sure that my physician colleagues and technologists are willing to accept the new standards of the protocol. Third, I must be sure that the new protocol is actually going to provide more efficient and effective care for the patients.
"A consistent skin marking protocol using distinct shapes for marking areas of interest on the breast not only offers radiologists the benefit of clearer communication helping to reduce misinterpretation, it also helps to save time when interpreting images.
"Additionally, consistently marking with this visual communication system aids patients by reducing call backs and potentially saving them from additional views and added radiation. All of which contribute to reducing the patient’s anxiety and enhancing the overall experience. "
The Beekley Skin Marking System® for Mammography offers breast imaging teams a simple way to document and identify these crucial findings as indicated by the ACR.
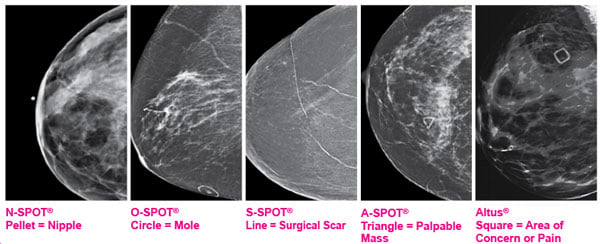
For decades, Beekley Medical® has been assisting radiologists in their diagnosis while reading mammograms with the 5-shape system of radiographically distinct skin markers. All our markers are raised and designed to be the least dense, allowing visualization underneath the marker so as not to hide tissue or obscure microcalcifications.
Triangle – the palpable mass marker: Represents the international sign of warning and has become a recognized universal industry symbol to indicate a palpable lump. Use of the triangle becomes a permanent record on the patient’s image, documenting the mass location.
Circle - to indicate a mole or raised skin lesion: Moles can image inconsistently from year to year and potentially mimic or be confused with a mass. They also may show up in one view but not the other, and 3D slices cannot always distinguish between a mole and mass. The O-SPOT® circular markers provide consistency and highlight raised lesions to distinguish what is on the skin line from what is below the surface.
Line – previous surgical scar: Linear markers subtly highlight the areas of a surgical scar. Due to the sensitivities of 3D Breast Tomosynthesis, architectural distortion is much more visible and more prevalent with benign excisions that may have been performed years earlier. Since many cancers reoccur at the site of a previous surgery, it is even more imperative to have a consistent visible notation on the radiographic image year after year.
Solid circle, pellet or BB - to indicate nipple location: For decades, technologists and radiologists were most familiar with their use to indicate a finding and were most relied upon to identify nipple location, due to burnout in the early days of film. Although 2D and 3D technology offer enhanced quality, the protocol of routine nipple marking continues to be especially beneficial. Statistics show that approximately 25% to 35% of cancers occur in the retroareolar region. Consistent use of nipple markers is advantageous for year to year comparisons and they serve as a permanent reference point to measure back to an area of concern.
Square - to denote non-palpable areas of concern or points of pain: Used most often to draw attention to concerns the patient communicates to the technologist. As opposed to using a triangle or a pellet which can cause confusion, the square offers a way to document the AOC with a clear distinct recognizable shape which is captured in the history of that patient’s images.
Beekley Medical is committed to providing the products that aid radiologists in their most accurate diagnosis. To learn more about the 5-shape Beekley Skin Marking System for Mammography and specific usage of the shapes in accordance with the ACR’s amended Practice Parameters, contact your Mammography Account Manager at 1-800-233-5539 or email info@beekley.com
For product safety information, visit beekley.com

Kathy Kaschuluk
Product Manager